Since July 1st ,2023, CalAIM/DHCS has released new changes in the CPT codes. We have provided a Outpatient MD Nurse Documentation Quick Guide (PDF) under the Prescriber, Nurses and Inpatient Tabs of CalMHSA’s website.
You can also find more information under Service Code Definitions which is broken down by role.
Of note, the Quick Guide information should be considered as high-level guidance, therefore specific scenarios should be conferred with your county billing administrators and/or contact [email protected] with your questions
Some considerations include:
- For face-to-face time, this is only for direct patient care which is defined when patient is present (unless the code specifically states that that patient does not need to be present when utilized).
- You can return within 24 hours of same service to amend that time if you had more discussion with patient/collateral beyond the original visit time.
- If service is completed or >24 hours, consider using another code that describes the interaction between patient/family and/or care team.
- The reimbursement is based on provider type, procedure code and face-to-face time.
- We recommend that you choose the code that best describes the type of interaction.
- For any codes that requires a certain # of minutes to be reimbursed, we still recommend that you choose the code that best describes the type of interaction for even if you don’t meet the reimbursement threshhold. Input the appropriate time spent, and let the system determine on the backend, whether the time is sufficient to be reimbursed.
- This is also recommended so that similar-like interactions can be found with the same procedure name and therefore, more easily discoverable when future teams are looking for your note and filtering based on procedure code.
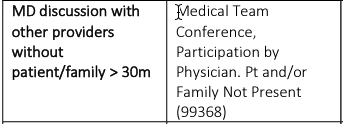
For example: Consider for any documented interactions between clinical team where patient care is discussed, using “Medical Team Conference” so that filtering by types of procedure codes is easier within the Services/Notes screen, even if that time is not reimbursed.